Frank Diamond | May 18, 2023
COVID-19 led to huge declines in care utilization, and insurers are still feeling the effects as they must dole out more than $1 billion in premium rebates this fall.
Payers will need to shell out about $1.1 billion in rebates, according to an analysis by the Kaiser Family Foundation based on data from state health insurance regulators compiled by Mark Farrah Associates.
Under the medical loss ratio rule in the Affordable Care Act, insurers must spend between 80% and 85% of their premium revenue on providing healthcare, with rebates based on the previous three years of experience. The three years previous to 2023—2020, 2021 and 2022—include the pandemic, when many providers didn’t offer routine care because they were too overloaded with COVID-19 patients, and many members decided to forgo care because of fear of being exposed to the virus.
The $1.1 billion figure may change, because some insurers have yet to file their rebate estimates, the researchers said. In addition, about two-thirds of covered workers belong to self-funded health plans, for which the MLR rule doesn’t apply.
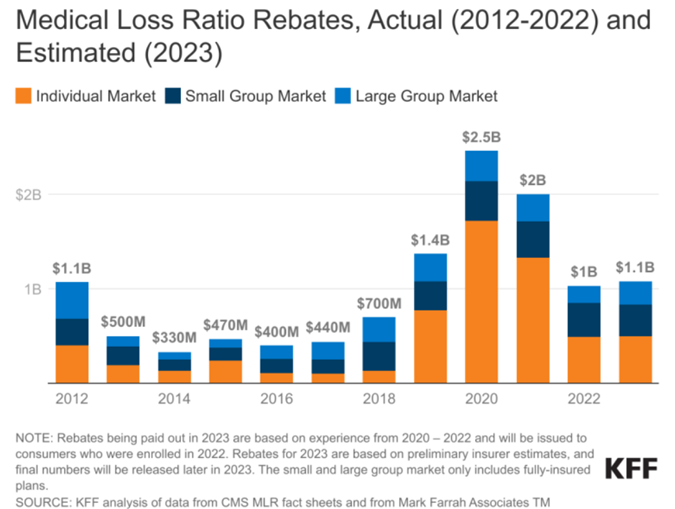
While the $1.1 billion that health insurers need to pay in rebates looms large, it is far less than the $2 billion that they paid in 2021 or the record-setting $2.5 billion that they paid in 2020, the peak of the pandemic.
Nonetheless, those numbers need to be put in context, Brad Ellis, senior director of North American insurance at the credit rating agency Fitch Ratings, told Fierce Healthcare.
“The health insurance sector in the U.S. in 2020 generated nearly a trillion dollars in premium revenue, and so $1.1 billion is not much in terms of the overall picture,” Ellis said. Though he noted that MLR rebates did jump substantially in 2020.
Also, there’s no denying that the pandemic caught the insurance industry off guard, Ellis said.
“The last time we had a pandemic was over 100 years ago,” Ellis said. “I think everyone, including us, didn’t realize how much utilization would go down. This surprised the entire healthcare industry, including providers.”
Source: Fierce Healthcare

